You all know about blood sugar and cholesterol. You probably think about your gut microbiome, your heart, and your brain.
But the organ quietly regulating all of them rarely crosses your mind.
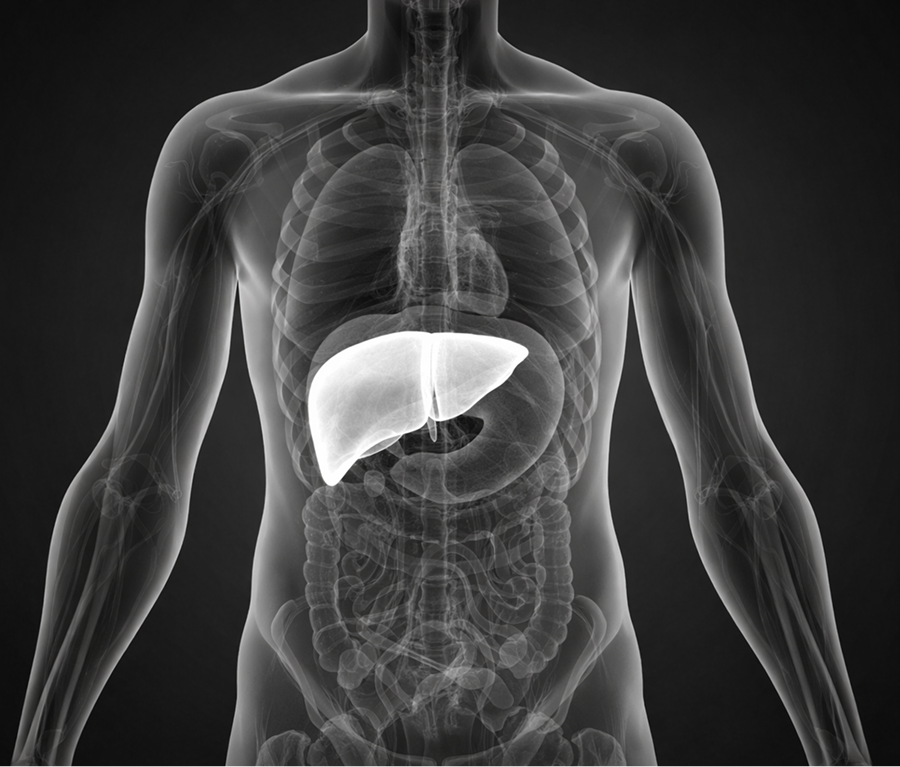
Your liver metabolizes every nutrient you eat. It filters toxins out of your bloodstream. It synthesizes many of the molecules your body runs on. And it sits at the center of the systems that control metabolism, energy, and long-term health.
But the liver doesn't announce itself. It doesn't beat or ache. It sits in the upper right of your abdomen, roughly three pounds, and works in silence, processing everything you eat, drink, breathe, and absorb through your skin. It synthesizes proteins that control blood clotting and support immune function. It stores and releases glucose to keep your energy stable between meals. It manufactures the cholesterol your cells need to build membranes, produce hormones, and synthesize vitamin D. It metabolizes every drug and supplement you take. It filters roughly 1.5 liters of blood per minute.
The liver performs over 500 known functions. It touches every major organ system in your body.
But right now, it's in serious trouble. Metabolic dysfunction-associated steatotic liver disease—MASLD, formerly known as non-alcoholic fatty liver disease (NAFLD)—has become the most common chronic liver condition in the world, affecting more than one in three adults globally. Liver disease is the ninth leading cause of death in the United States. Most of this damage accumulates silently (no symptoms, no pain, no warning).
So many of the conversations we're already having in this newsletter about metabolic health, blood sugar, cholesterol, and longevity all run through the liver.
What Your Liver Did Today
Before you got out of bed this morning, your liver had already been working for hours.
While you slept, it regulated your blood sugar, releasing stored glucose in careful, measured doses to keep your brain fueled and your blood sugar stable through the night.
It filtered roughly 720 liters of blood, clearing metabolic waste, deactivating hormones that had done their job, and neutralizing whatever residual toxins were still circulating from the day before.
It produced bile and stored it in your gallbladder, ready to deploy the moment you eat your first meal.
It synthesized albumin and clotting factors, proteins your blood needs to maintain pressure and stop bleeding. It continued processing and repackaging cholesterol into lipoproteins for distribution across your body.
Then you woke up, ate breakfast, drank coffee, maybe took a supplement or a medication—and your liver absorbed every bit of it. It extracted nutrients from what you ate and sent them where they needed to go. It metabolized the caffeine. It processed the active compounds in your supplement.
This is what 500 functions looks like in practice.
A Message from Our Partner
How much attention do you actually give your liver?
That question matters more than most people realize. Your liver is one of your body's most important organs. Metabolic dysfunction associated fatty liver disease (MASLD) now affects nearly 40% of adults in the Western world, often developing long before people notice symptoms.
It doesn't get as much care and attention as your heart, your gut, or your brain. But it should.
That’s the idea behind de-liver-ance®, a natural antioxidant elixir developed over two decades to support liver health. It blends plant extracts, herbal compounds, and honey into a daily tonic designed to improve all 500+ functions your liver performs daily, so you can have better skin, a stronger immune system, and more mental clarity. Because when the liver functions well, many other things improve.
And if you’re curious how your liver is actually doing, The Liver Clinic will offer FibroScan® testing at this year's Eudēmonia Summit. FibroScan® is a quick, non-invasive scan that measures liver fat and stiffness, allowing you to see real data about your liver health and track progress over time.
Get 20% off your first order using the code: Eudemonia.
Your Liver Makes Cholesterol
Here's a fact that still surprises people: your liver produces roughly 80% of the cholesterol in your body. Only about 20% comes from what you eat.
Every day, your liver takes basic metabolic building blocks from the food you consume and turns them into cholesterol. It then packages that cholesterol into transport particles called lipoproteins and sends them through your bloodstream to the cells that need it.
Because cholesterol isn’t optional; it’s essential. Every cell membrane in your body depends on it. Your body uses it to produce bile acids that digest fat. It’s the raw material for steroid hormones like testosterone, estrogen, and cortisol. And it’s the precursor your skin uses to manufacture vitamin D from sunlight.
Without cholesterol, your biology simply doesn’t run. So the molecule itself isn’t the problem. The problem begins when the liver’s systems for producing, transporting, and clearing cholesterol fall out of balance.
This is where the story gets interesting.
Your liver packages the cholesterol it produces into transport particles called very-low-density lipoproteins (VLDL) and releases them into your bloodstream. As these particles circulate through the body, they deliver triglycerides to tissues that need energy. As they lose those triglycerides, they shrink and become denser, eventually turning into LDL.
That’s the number your doctor flags on your annual blood test. And most of it didn’t come from what you ate that morning. It came from your liver.
Now here’s the key link.
When you consistently eat more sugar than your body can easily handle, insulin signals the liver to ramp up fat production and release more VLDL. More VLDL moving through the bloodstream eventually means more LDL downstream.
This is why metabolic dysfunction—insulin resistance, elevated blood sugar, excess visceral fat—is so tightly linked to abnormal cholesterol levels. They aren’t separate problems. They’re different expressions of the same metabolic imbalance.
Meanwhile, HDL particles move in the opposite direction. They collect excess cholesterol from the bloodstream and return it to the liver for recycling or removal. That process is called reverse cholesterol transport. And it only works well when the liver is healthy enough to do its job.
Your cholesterol panel is, in many ways, a liver function report. If you want to understand why those numbers are what they are, look at the organ making the decisions.
Your Liver and Your Blood Sugar
Your liver is a major glucose reservoir that helps keep blood sugar in a healthy range, storing glucose after meals and releasing it between meals under the direction of hormones like insulin and glucagon. After you eat, rising blood sugar triggers insulin, which tells the liver to stop releasing glucose and start storing the excess as glycogen (and, if there’s more than it can store as glycogen, to turn some into fat), a kind of short term energy reserve.
Later, when you haven’t eaten for a while, the signal flips. Blood sugar begins to fall and the liver releases some of that stored glucose back into the bloodstream to keep things stable. This is why your brain stays fueled even when you go hours without eating.
When the system is healthy, the liver is constantly making these small adjustments. Store a little. Release a little. Keep the level steady.
Insulin resistance is what happens when the liver stops listening properly to insulin’s instructions. After a meal, insulin says “stop releasing sugar.” But the liver ignores the message and keeps sending glucose into the bloodstream anyway.
Now blood sugar rises higher than it should. The pancreas responds by releasing even more insulin to attempt to take control of the situation. High insulin pushes more energy into storage and encourages fat to accumulate in the liver itself.
And here is the problem: a liver that accumulates fat becomes even more resistant to insulin. So the cycle feeds on itself.
The liver releases too much sugar → blood sugar rises → insulin rises → fat builds up in the liver → the liver becomes even more insulin resistant
In reality, the cycle can start at more than one point. In many people, fat begins accumulating in the liver first, which then triggers the insulin resistance that drives the rest of the loop.
Over time, that loop can lead to fatty liver disease, type 2 diabetes, and many of the metabolic problems people associate with aging. Which is why blood sugar is not just a pancreas story. A large part of it is a liver story.
How Fat Starts Building Up in the Liver
Fat doesn’t build up in the liver overnight. It accumulates gradually when there’s more fuel coming in than the body can burn or safely store in fat tissue. The liver is one of the body’s main fuel processors: when energy keeps arriving in excess, especially in the form of sugars and fats, it converts some of that surplus into fatty acids and packages them as tiny fat droplets inside liver cells.
Over time, if this imbalance continues, those droplets accumulate and the liver becomes increasingly loaded with fat.
Fructose plays a role as well. Fructose—the sugar found in fruit, table sugar, and many sweetened foods and drinks—is metabolized largely in the liver. Unlike glucose, which can be used directly by many tissues around the body, a substantial share of fructose is taken up and processed there. When fructose comes in large or frequent amounts, especially on top of excess calories, the liver converts more of it into fat, which can contribute to fat buildup in the liver over time.
Refined carbohydrates contribute in a different way. Foods like white bread, pastries, and sugary snacks quickly spike blood sugar and insulin, which nudges the liver to turn more of that excess sugar into fat.
Fat can also arrive from another direction. When fat cells release fatty acids into the bloodstream, the liver takes up part of that flow. If this incoming supply stays high enough for long enough, more of those fatty acids are converted into triglycerides and stored inside liver cells.
Genetics matter too. Some people inherit liver traits that make them more likely to accumulate fat, even when their body weight is normal. In these cases, the problem isn’t always how much fat the liver makes, but how well it handles and exports it. Normally, the liver packages triglycerides into particles called VLDL and ships them into the bloodstream. When this export system can’t keep up with the fat coming in and being made, more fat is left behind and begins to build up inside the liver itself.
Once enough fat builds up inside liver cells, it can interfere with the liver’s ability to “hear” insulin properly, contributing to hepatic insulin resistance. When that happens, the liver keeps releasing glucose even when insulin is high, forcing the pancreas to pump out more insulin and locking in a vicious cycle where high glucose, high insulin, and liver fat keep driving each other.
What Goes Wrong
Metabolic Dysfunction–Associated Steatotic Liver Disease (MASLD) ( Formerly called NAFLD)
MASLD begins with fat accumulating in the liver. Over time, that extra fat can set off inflammation and steatohepatitis, then scarring (fibrosis), cirrhosis, and even liver cancer in a subset of people. The condition now affects roughly one in three adults in the United States, and among people with type 2 diabetes, it’s seen in about two‑thirds.
What makes MASLD particularly dangerous is that most people have no obvious symptoms. No pain, no clear fatigue, nothing that would automatically send you to the doctor. The disease can quietly progress for years before it’s picked up on blood tests or imaging. And it’s not only a disease of obesity—a distinct “lean MASLD” phenotype occurs in people with normal body weight, driven more by insulin resistance, visceral fat around the organs, and inherited liver‑fat risk genes
Alcohol-Related Liver Disease (ALD)
ALD is liver damage caused by long‑term heavy drinking, ranging from fatty liver to hepatitis, fibrosis, cirrhosis, and liver cancer. Alcohol and its toxic metabolite acetaldehyde directly injure liver cells, drive oxidative stress, and promote inflammation and scarring.
When this sits on top of metabolic dysfunction—things like obesity, insulin resistance, or MASLD—the risks compound: metabolic disease makes the liver more vulnerable to alcohol at lower doses, and alcohol worsens fat build-up and inflammation in an already stressed liver, so together they accelerate progression to advanced liver disease.
Viral Hepatitis
Hepatitis B and C remain major causes of cirrhosis and liver cancer globally, particularly in parts of Africa and Asia where vaccination and treatment are less accessible.
Drug-Induced Liver Injury
Certain medications and supplements can also injure the liver. Because the liver is the body’s main processing center for many drugs, chemicals, and herbal compounds, it is especially vulnerable to damage when these substances—or their reactive breakdown products—are present in high amounts or in susceptible individuals.
Despite their different triggers, many liver diseases end up following a similar path. Healthy tissue is slowly replaced by scar tissue; at its most advanced stage, this scarring is called cirrhosis. Once cirrhosis develops, the liver’s remarkable ability to regenerate starts to fail, and complications like fluid buildup, internal bleeding, cognitive changes, liver cancer, and other problems become more likely.
By that point, the quiet system that has supported your metabolism for decades has been pushed beyond its limits.
Keeping It Healthy
Here's the good news: the liver responds remarkably well to intervention, especially early. Fatty liver disease—even with moderate scarring—is reversible with sustained lifestyle changes. The same metabolic levers that drive liver disease can be pulled in the other direction. Here's what the evidence supports.
Move.
Exercise is one of the most reliable ways to improve liver health, and it works even without weight loss. The two forms that matter most are Zone 2 cardio and resistance training.
Zone 2 cardio means steady, moderate effort. Brisk walking, cycling, jogging, rowing. The kind of pace where you can still talk but your breathing is elevated. This type of training improves insulin sensitivity and helps your body burn fat more efficiently, which reduces the amount of fat building up in the liver.
Resistance training helps in a different way. Muscle is one of the body’s main places to store and use glucose. The more muscle you build, the more capacity your body has to absorb sugar from the bloodstream instead of forcing the liver to manage it.
You don’t need extreme protocols. Research shows meaningful improvements with about 150 minutes of moderate activity per week, along with a few sessions of strength training.
Eat for your liver.
Start by dialing back refined sugar and excess fructose. This is one of the highest-impact dietary changes you can make. Fructose is processed almost entirely by the liver, and in large amounts it pushes the liver to convert that sugar into fat. That’s why high-fructose corn syrup and fruit juice tend to be particularly problematic.
Next, prioritize fiber. Higher fiber intake improves insulin sensitivity and feeds beneficial gut bacteria that produce short‑chain fatty acids, which help calm inflammation, improve glucose handling, and support healthier liver metabolism through the gut–liver axis. A healthier gut barrier means fewer inflammatory and microbial signals reaching the liver. Cruciferous vegetables like broccoli, Brussels sprouts, kale, and cauliflower are especially helpful; they provide compounds such as sulforaphane and indole‑3‑carbinol that support detoxification and antioxidant defenses in the liver
And then there’s coffee. The research here is surprisingly consistent: regular coffee consumption is associated with lower risks of liver fibrosis, cirrhosis, and liver cancer, along with better liver enzyme profiles in people with and without chronic liver disease. Benefits appear to come from antioxidant, anti‑inflammatory, and anti‑fibrotic effects of coffee’s bioactive compounds. Across meta‑analyses, roughly 2–3 cups per day is the range most often linked with meaningful protection, with some studies suggesting additional benefit at slightly higher intakes for certain outcomes
Some people also add a tablespoon of apple cider vinegar diluted in water before meals. Early studies suggest it may blunt post-meal blood sugar spikes—a small metabolic nudge that can indirectly support liver health over time.
Moderate alcohol.
There's no magic threshold below which alcohol is completely safe for the liver, but the dose-response relationship is clear: less is better. If you already have any degree of fatty liver, insulin resistance, or metabolic dysfunction, the threshold for alcohol-related harm drops significantly.
Monitor.
Standard liver enzyme panels—ALT, AST, and GGT—are inexpensive, widely available, and included in most basic metabolic blood work.
They're imperfect: you can have significant fatty liver with completely normal enzymes, and a single elevated reading doesn't tell you much on its own. But trends matter. A gradual upward drift in ALT over several years is worth investigating.
Elevated GGT in particular is an underappreciated marker. Higher GGT levels correlate with fatty liver, metabolic stress, and oxidative injury, and even within the “normal” range, they’re associated with increased risks of cardiovascular disease and all‑cause mortality, independent of alcohol use.
For people at higher risk—those with obesity, type 2 diabetes, insulin resistance, or a family history of liver disease—more sensitive screening tools exist. Ultrasound‑based elastography (often called FibroScan) can non‑invasively assess both liver stiffness (fibrosis) and fat content. The FIB‑4 index, a simple calculation using age, ALT, AST, and platelet count, can stratify fibrosis risk from routine labs and help identify who needs further work‑up. These aren’t exotic tests; they’re increasingly available in primary care and liver clinics and are worth asking about if you’re in a higher‑risk group.
Supplement thoughtfully.
No supplement replaces the fundamentals above. But a few compounds have meaningful evidence for supporting liver health.
Milk thistle is the classic one. Its active compound, silymarin, has been studied for decades and shows anti-inflammatory, antioxidant, and anti-fibrotic effects in liver tissue.
NAC (N-acetylcysteine) works in a different way. It helps your body produce glutathione, the liver’s primary antioxidant defense. In hospitals, NAC is actually used as the treatment for acetaminophen overdose because it protects liver cells from damage.
Omega-3 fatty acids, particularly EPA and DHA, can also help. They lower triglycerides and have been shown to reduce liver fat in people with metabolic liver disease.
Other compounds like berberine, curcumin, and phosphatidylcholine are being studied as well. The research is still early, but the results suggest additional ways these molecules may support liver metabolism and inflammation.
Supplements can help. But they work best when the foundation—diet, movement, sleep, and alcohol moderation—is already in place.
The Liver and Longevity
In longevity science, we often talk about the biological forces that slowly wear the body down—accumulating DNA damage, mitochondrial dysfunction, cellular senescence, and chronic inflammation.
The liver touches nearly all of them.
It clears metabolic waste. It regulates inflammatory signals that drive the slow, chronic inflammation often called inflammaging. It produces and clears the lipoproteins that influence cardiovascular risk.
And it governs blood sugar regulation, one of the strongest predictors of aging and age-related disease.
When liver function begins to decline, even slightly, the effects ripple through the entire system.
Detoxification slows. Oxidative stress rises. Cholesterol clearance weakens. Blood sugar regulation deteriorates. Insulin resistance begins to creep in.
None of this usually announces itself dramatically, and the liver rarely fails all at once. Instead, it gradually erodes the body’s systems. This is why liver health is a longevity issue—not just a disease-avoidance issue.
The difference between a liver functioning at 90% and one functioning at 60% may not appear on a standard blood panel. But it shows up in how you age: your energy, your recovery, your metabolic flexibility, and your ability to handle decades of stress.
It’s not talked about enough in the modern wellness conversation.
But if you care about longevity and sustaining vitality across decades, your liver deserves the same attention you give your heart, brain, gut, and whatever else you’re focusing on. If you catch liver problems early on, they can be reversible. But if you don’t discover them until very late, it will be difficult.
Pay more attention to it now, so you have fewer (or zero) problems later.
Disclaimer: This newsletter is provided for educational and informational purposes only and does not constitute providing medical advice or professional services. The information provided should not be used for diagnosing or treating a health problem or disease, and those seeking personal medical advice should consult with a licensed physician.

March 27, 2026
March 21, 2026

March 13, 2026

March 6, 2026

February 28, 2026
February 21, 2026

February 14, 2026

February 7, 2026

January 23, 2026